 Future Performance Training
Future Performance Training
Heat illness follows a continuum. In other words, after the onset of a minor heat illness (if left uncared for), major heat illness will result. It is important to recognize and treat the symptoms of heat illness early to prevent a victim from progressing to heat stroke. In all heat emergencies you will first need to cool the victim down.
|
Heat Cramps |
Heat Exhaustion |
Heat Stroke |
|
- Severe muscle cramps - Moist, cool skin - Heavy sweating.
- Remove casualty to a cool place. - Give casualty water with salt/ rehydration fluid. - Pull on cramped muscle. - Massage muscle.
|
- Skin ‑ flushed, cold and clammy - Heavy sweating - Pulse ‑ weak - Headache - Breathing ‑ Rapid and - Shallow - Nausea - Stomach cramps - Weakness, fatigue
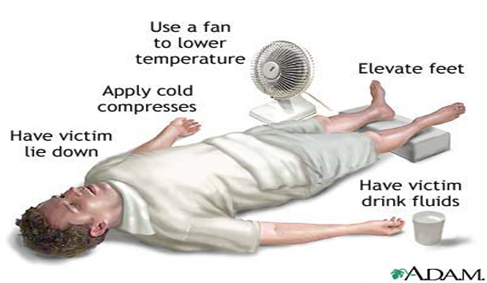
- Remove casualty to a cool place. - Elevate legs. - Remove unnecessary clothing. - Apply cool packs. - Give water. - Monitor!
|
- Skin ‑ Dry, hot and red - LOC decreased - Little or no sweating - Pulse ‑ full, rapid.
- Remove casualty to a cool place. - Remove unnecessary clothing. - Sprinkle the casualty with continuously flowing water. - Fan the casualty to further cool him/ her down. - Call EMRS! (Life-threatening) |
Hypothermia
Hypothermia is the general cooling of the body. It can start off mild and, if uncared for, will develop into severe hypothermia which is life-threatening. The sooner you recognize the signs of hypothermia and provide care, the better the chance is that the condition will not progress. In water the body looses heat 21 times faster than the air at the same ambient temperature. In either case, SEEK MEDICAL ATTENTION!! Never give victim alcohol or caffeine to drink!

Signs and Symptoms
- Body core temperature 37 oC .... >35 oC
- Shivering
- Slurred speech
- Stumbling or staggering
- Usually the patient is conscious and can talk
First Aid Care
- Removal from cold environment
- Have a source of heat (warm water, fire place)
- Replace wet clothing with dry
- Provide a hat, blankets, coats, etc. Insulate victim
- Seek medical attention.
Moderate to Severe Hypothermia
Signs and Symptoms
- Body core temperature <35 oC
- Shivering has stopped
- Muscles have become stiff and rigid
- Skin has a bluish appearance
- Skin does not react to pain
- Respiration and pulse slow down
- Pupils will dilate
- Victim may appear dead
- Decreased level of consciousness
- Failing eye sight.
First Aid Care
- Remove patient from cold environment
- Remove any wet clothing and replace with dry clothing
- Passively re-warm the patient (>35oC) ‑ Wrap in a space blanket and give him/her warm drinks (if conscious)
- Have a source of heat (warm water, fire place)
- Provide a hat, blankets, coats, etc. Insulate victim
- Seek medical attention.
Special Care
Children and elderly patients may be more susceptible to hypothermia and may not show the same signs and symptoms. Children have a low body fat. Older patients may have a higher susceptibility due to loss of fat and decreased efficiency in maintaining normal body temperature.
Drowning is defined as death by suffocation under a fluid medium whilst near drowning may be defined as survival following asphyxia or aspiration due to submersion in a fluid medium.
- WET AND COLD!!
- No responsiveness
- No Breathing
- Cyanosis
- Froth around the casualty's mouth and nostrils
- Pupils ‑ Dilated and fixed
- Loss of vital signs.
- SAFETY! ‑ Throw, tow, row then go, if trained to do so.
- Assess the vital signs.
- CPR, if necessary ‑ CPR is not possible in water. Ventilate the casualty and then move him/ her onto the side of the pool or shore or into a boat. Commence with CPR. With cold water drowning continue with CPR until the EMS arrives.
“A CASUALTY IS NOT DEAD UNTIL WARM AND DEAD”



INHALATION INGESTION INJECTION
Many of the signs and symptoms of poisonings are the same.
- Difficulty breathing.
- Abdominal pain.
- Headache.
- Nausea and vomiting.
- Neurological dysfunction.
- Excessive salivation and sweating.
- LOC changes (drowsiness ......unconsciousness/ coma).
- Burns, stains and odour in and around the mouth and lips.
|
1 |
Asses the scene for clues and safety. Get patient away from poison, if necessary. |
|
2 |
Assess victim response (Vital Signs) |
|
3 |
Provide care for any life-threatening conditions |
|
4 |
If patient is conscious, attempt to get more information. |
|
5 |
Contact Poison Information Centre or local EMRS. Bring any empty container, plant, etc ... to the phone for verification purposes. |
|
6 |
Follow treatment instructions of Poison Centre |
Do not induce vomiting in the following cases:
- Unconscious or disorientated patients.
- Petroleum/ Paraffin products where ingested.
- Acids/ Alkalis were induced.
- Convulsions.
- Children younger than 1 year old.
- Rattex / similar products ingested.
There are literally thousands of species of insects capable of stinging. Fortunately, most are not considered to be dangerous. If a stinging victim develops serious symptoms including shortness of breath, flushing, swelling of the face or severe swelling of a body part, further medical attention should be sought immediately. A severe reaction could mean a life-threatening condition is developing - namely, anaphylaxis.

Bees are the only insects that will leave behind a stinger that may remain embedded in the skin. Remove the sting by scraping the sting out with a blade in opposite direction to what the sting is laying. Try not to damage the poison sac. Apply anti‑histamine cream and monitor the patient for allergic reaction.

Touch the tick with a lit cigarette and it will fall off accordingly. Alternatively you can apply oil over the tick. The oil closes the breathing pores and the tick falls off. Clean the area with soap and water, apply anti‑histamine cream. If you are unable to remove the head or if rash persist, obtain medical assistance.

Try collect/ identify the spider. Disinfect the bite. Apply ice to the bite. Bandage the limb ‑ Distal to proximal. Immobilise the limb.

SCORPIONS
Apply ice pack immediately. Disinfect the sting area. Apply ice to the bite. Bandage the limb‑ Distal to proximal. Immobilise the limb. Monitor the patient for allergic reaction.
SAFETY!! CABC Identify the snake, if possible. Reassure the casualty ‑ keep casualty calm. Bandage the limb, using a firm crepe bandage. Bandage the whole limb, from below the bite wound and towards the heart (distal to proximal). Beware with puff‑adder bites due to severe tissue damage and swelling. Should snake venom land in the eyes, rinse thoroughly with a non irritating liquid (e.g. water). Immobilise the casualty (i.e. patient must not move).
